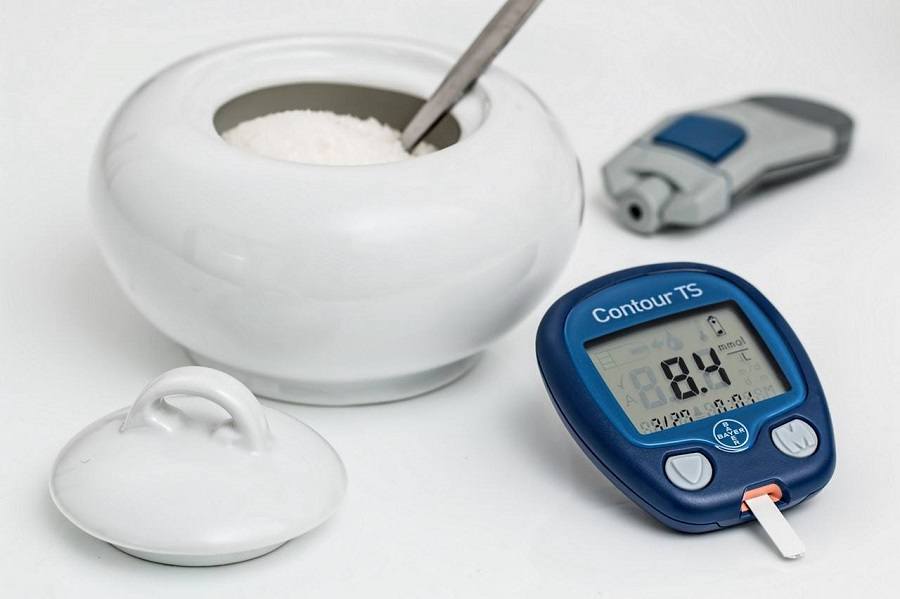
The blood sugar concentration or blood glucose level is the amount of glucose (sugar) present in the blood of a human or an animal. The body naturally tightly regulates blood glucose levels (with the help of insulin that is secreted by pancreas) as a part of metabolic homeostasis.
If blood sugar levels are either increased or decreased by a greater margin than expected this might indicate a medical condition.
Diabetic patients must monitor their levels as body’s inability to properly utilize and / or produce insulin can pose a serious threat to their health.
Navigation:
Definition:
What is blood sugar?
What is diabetes?
Diagnosis:
Diabetes symptoms
Levels and indication
Normal levels
Low levels
High levels
Managing:
How to lower blood sugar level?
Children blood sugar levels
Blood sugar levels chart
Checking for BS:
How to check blood sugar?
Treatment:
How to lower blood sugar level?
Can diabetes be cured?
Accessories
Diabetic Socks
Diabetic Shoes
What is blood sugar?
Blood sugar level (or blood sugar concentration) is the amount of glucose (a source of energy) present in your blood at any given time.
A normal level for a healthy person is somewhere between 72 mg/dL (3.8 to 4 mmol/L) and 108 mg/dL (5.8 to 6 mmol/L). It, of course, depends on every individual alone. Blood sugar levels might fluctuate due to other reasons (such as exercise, stress and infection).
Typical levels in humans is around 72 mg/dL (or 4 mmol/L). After a meal the blood sugar level may increase temporarily up to 140 mg/dL (7.8 mmol/L). This is normal.
A blood sugar level between 72 mg/dL (4 mmol/L) and 108 mg/dL (6 mmol/L) is considered normal for a healthy adult.
Note: mg/dL and mmol/L are units of measure. mg/dL is mostly used in USA whereas mmol/L is mostly used in EU and other parts of the world. For easier conversion try our mg/dL mmol/L conversion tool.
What is normal blood sugar level?
Adults
For a healthy adult a normal level is between 72 mg/dL and 108 mg/dL (4 to 6 mmol/L). The concentration of glucose in the blood of a healthy person in the morning on an empty stomach is between 68 mg/dL and 108 mg/dL (3.8 and 6.0 mmol/L). Two hours after consuming foods or drinks rich in carbohydrates, the values are usually between 120 and 140 mg/dL (6.7 and 7.8 mmol/L).
Children
For children up to 6 years of age desired level before eating is between 100 mg/dL (5.5 mmol/L) and 180 mg/dL (10 mmol/L). Before sleep values should be between 110 mg/dL (6.1 mmol/L) and 200 mg/dL (11.1 mmol/L).
For children between the age of 6 and 12, before eating, blood sugar levels should be between 90 mg/dL (5 mmol/L) and 180 mg/dL (10 mmol/L). Before sleep values should be between 100 mg/dL (5.5 mmol/L) and 180 mg/dL (10 mmol/L).
Children aged 13 to 19 should expect similar readings than those of adults.
Blood sugar levels chart
Blood sugar levels rise and drop during the day. This is normal. However, dramatic fluctuations in your blood glucose levels may indicate problems.
Dramatic changes of blood sugar levels have significant physical symptoms and will increase your risk of diabetes-related complications.
Click on the image below to view a larger blood sugar levels chart.

Download your blood sugar levels log and keep track of your results – write down all of your measured values.
| Glucose mg/dL or mmol/L | Value |
|---|---|
| Before breakfast (fasting) | 70 – 130 mg/dL or 3.9 – 7.2 mmol/L |
| Before lunch, supper and snack | 70 – 130 mg/dL or 3.9 – 7.2 mmol/L |
| Two hours after meals | less than 180 mg/dL or less than 10mmol/L |
| Bedtime | 90 – 150 mg/dL or 5 – 8.3 mmol/L |
| A1C (also called glycosylated hemoglobin A1c, HbA1c or glycohemoglobin A1c) | less than 7% |
Please note that you should perform several consecutive blood glucose tests and not rely on one single measurement.
The next chart displays all possible blood sugar (glucose) levels along with a short explanation of what the indicators are.
| Blood Sugar Levels | Indication |
|---|---|
| Less than 70 mg/dL (3.9 mmol/L) | Low fasting blood sugar |
| 70 to 108 mg/dL (3.9 to 6 mmol/L) | Normal fasting blood sugar for adults |
| 110 to 125 mg/dL (6.1 to 6.9 mmol/L) | Impaired fasting glucose (pre-diabetes) |
| 126 mg/dL (7.0 mmol/L) and above in more than one test result | Diabetes |
| about 70 to 140 mg/dL (3.9 to 7.8 mmol/L) | Normal postprandial blood sugar |
| about 142 to 199 mg/dL (7.9 to 10.9 mmol/L) | Borderline postprandial blood sugar. May indicate pre-diabetes. |
| Less than 70 mg/dL (3.9 mmol/L) | Hypoglycemia (Initial Stage) |
| 50 mg/dL (2.8 mmol/L) | Hypoglycemia (Fasting) |
| less than 50 mg/dL (2.8 mmol/L) | Insulin Shock |
| 145 – 200 mg/dL (8 – 11 mmol/L) Post meal | Value suggesting early diabetes |
| More than 200 mg/dL (11 mmol/L) Post meal | Value suggesting established diabetes |
Normal values for blood sugar are (values are in mmol/L, mg/dL and HbA1c) in the table below.
| Blood sugar levels | HbA1c | mg/dL | mmol/L |
|---|---|---|---|
| low | less than 4 | less than 65 | less than 3.6 |
| normal optimal | 4 | 65 | 3.6 |
| normal optimal | 4.1 | 69 | 3.8 |
| normal optimal | 4.2 | 72 | 4 |
| normal optimal | 4.3 | 76 | 4.2 |
| normal optimal | 4.4 | 80 | 4.4 |
| normal optimal | 4.5 | 83 | 4.6 |
| normal optimal | 4.6 | 87 | 4.8 |
| normal optimal | 4.7 | 90 | 5 |
| normal optimal | 4.8 | 94 | 5.2 |
| normal optimal | 4.9 | 97 | 5.4 |
| good marginal | 5 | 101 | 5.6 |
| good marginal | 5.1 | 105 | 5.8 |
| good marginal | 5.2 | 108 | 6 |
| good marginal | 5.3 | 112 | 6.2 |
| good marginal | 5.4 | 115 | 6.4 |
| good marginal | 5.5 | 119 | 6.6 |
| good marginal | 5.6 | 122 | 6.8 |
| good marginal | 5.7 | 126 | 7 |
| good marginal | 5.8 | 130 | 7.2 |
| good marginal | 5.9 | 133 | 7.4 |
| at risk | 6 | 137 | 7.6 |
| at risk | 6.1 | 140 | 7.8 |
| at risk | 6.2 | 144 | 8 |
| at risk | 6.3 | 147 | 8.2 |
| at risk | 6.4 | 151 | 8.4 |
| at risk | 6.5 | 155 | 8.6 |
| at risk | 6.6 | 158 | 8.8 |
| at risk | 6.7 | 162 | 9 |
| at risk | 6.8 | 165 | 9.2 |
| at risk | 6.9 | 169 | 9.4 |
| dangerously high | 7 | 172 | 9.6 |
| dangerously high | 7.1 | 176 | 9.8 |
| dangerously high | 7.2 | 180 | 10 |
| dangerously high | 7.3 | 183 | 10.2 |
| dangerously high | 7.4 | 187 | 10.4 |
| dangerously high | 7.5 | 190 | 10.6 |
| dangerously high | 7.6 | 194 | 10.8 |
| dangerously high | 7.7 | 198 | 11 |
| dangerously high | 7.8 | 201 | 11.2 |
| dangerously high | 7.9 | 205 | 11.4 |
| possible complications | 8 | 208 | 11.6 |
| possible complications | 8.1 | 212 | 11.8 |
| possible complications | 8.2 | 215 | 12 |
| possible complications | 8.3 | 219 | 12.2 |
| possible complications | 8.4 | 223 | 12.4 |
| possible complications | 8.5 | 226 | 12.6 |
| possible complications | 8.6 | 230 | 12.8 |
| possible complications | 8.7 | 233 | 13 |
| possible complications | 8.8 | 237 | 13.2 |
| possible complications | 8.9 | 240 | 13.4 |
| mortal danger | 9 | 244 | 13.6 |
| mortal danger | 9+ | 261+ | 13.6+ |
What is considered low blood sugar level?
When your blood sugar level drops below 70 mg/dL (3,9 mmol/L) this means you have a low level of blood sugar. The usual symptoms are:
- hunger,
- sweating,
- restlessness,
- faltering speech,
- confusion,
- tremor,
- difficulty in concentration,
- drowsiness,
- headache,
- visual disturbances…
Symptoms may vary – different people might experience different symptoms. In some cases symptoms can even remain unrecognized (unconscious hypoglycemia).
What is considered high blood sugar level?
Chronically high blood sugar (diabetes) is caused by a number of abnormalities in the body, one of them being the affected vascular walls of small and large arteries (diabetic micro-and macro-angiopathy) in a process called atherosclerosis.
We can say that a blood sugar level is high if we measure glucose level and get the following values – more than 110 mg/dL (6.1 mmol/L) on an empty stomach or at any time more than 200 mg/dL (11.1 mmol/L).

High blood sugar levels affect the arteries throughout the body, especially the organs which have the richest blood circulation: heart, brain, kidney, senses, nerves and other organs.
If the high blood sugar is associated with disturbances in lipid metabolism (blood fat), the abnormalities are more intense. Diabetes is among the risk factors for major non-communicable diseases: cardiovascular (coronary) disease, cerebral vascular disease and peripheral vascular diseases.
Diabetes symptoms
Typical symptoms of high blood sugar levels (diabetes) are thirst, frequent urination and unexpected weight loss. Sometimes a patient may also experience the following:
- impaired vision,
- itching skin,
- fatigue,
- increased appetite,
- skin infections,
- feeling of dizziness,
- heavy dehydration.
Type 1 diabetes symptoms are severe and last for a short time before the disease is diagnosed. Type 2 diabetes symptoms appear slowly and are usually unrecognizable or nearly absent.
Use this tool to convert blood sugar values.
How to check blood sugar
There are basically two main tests which are conducted to determine whether someone has diabetes.
Impaired fasting glycemia test
When being tested for diabetes by a impaired fasting glycemia test, blood sugar levels will normally be taken after around eight hours of fasting.
Impaired glucose tolerance test
An impaired glucose tolerance test involves taking a concentrated amount of glucose and then measuring blood sugar levels after two hours.
In a healthy person, a normal blood glucose level is between 72 mg/dL (4 mmol/L) and 108 mg/dL (6 mmol/L). Read on how to check blood sugar values.
For checking your blood sugar level, you will need:
Medical alcohol to clean the skin where you will prick your finger, a sterile tool to prick your finger, some test strips and a glucose meter to read the test strip.
| Glucose mg/dL or mmol/L level | Value |
|---|---|
| less than 110 mg/dL or 6 mmol/L on an empty stomach | normal value |
| between 110 mg/dL or 6.1 mmol/L and 125 mg/dL or 6.9 mmol/L on an empty stomach | limit value |
| more than 125 mg/dL or 7.0 mmol/L on an empty stomach | possible diabetes |
| more than 198 mg/dL or 11.0 mmol/L anytime | possible diabetes |
Can diabetes be cured?
At this time there is no known official case of cured diabetes, however with proper action (diet and exercise), type 2 diabetes can be suppressed, but never reverted. There is no known case of diabetes type 1 recovery. Gestational diabetes (high blood sugar levels that manifest during pregnancy) will revert after pregnancy, but might develop into Diabetes Type 2 later in life.
Why diabetes type 1 cannot be reversed
With Diabetes type 1 body’s cells that produce insulin are destroyed. These cells cannot be regrown or replaced. A person would need to use insulin injections to control their condition.
With type 2 diabetes your body does not use insulin properly (also known as insulin resistance). Over the time a patient’s condition worsens as body cannot make enough insulin to keep blood glucose at normal levels.
How to keep diabetes under control?
In addition to modifying your diet, walk for 10 minutes after each meal to help improve insulin sensitivity and glucose uptake into your cells. Eat quality food and monitor your carbohydrates. Get a referral to a certified diabetes educator who will modify their recommendations based on your body, not what the guidelines say. If your blood sugar is still high with the recommended amount of carbs per meal, decrease the carbs further. Avoid low fat foods. Fat and protein will help your body absorb carbs more slowly and prevent spikes and troughs in your blood sugar.
Since diabetic diet is restrictive, you should change your view from focusing on the things you can’t eat to focusing on all of the delicious things you can eat. All food groups are still on the table. You may have to modify recipes but there are so many awesome alternatives to almost any food available on the internet.
It is recommended to severely decrease your daily carbohydrates intake. However Low carb diets can still be rich and delicious.
Diabetics are recommended to avoid certain types of fruit, however, in moderation, all kinds of fruits can still be consumed. They key is to eat them in moderation. For example, half a banana is already one serving of carbohydrates. Apples and oranges should be no larger than a tennis ball. Be careful with dried fruits because they are concentrated.
List of foods that raise blood sugar levels
High Glycemic index foods
Certain foods will make your blood sugar go up quite rapidly. These foods are known as s high-glycemic foods. See more on glycemic index.
Avoid eating foods that are high on the glycemic index (bananas, pineapple, watermelon and dried fruits, carrots, white potatoes and beets, and corn – this means high fructose corn syrup, so virtually all packaged foods). Eat fresh fruit with skins at the beginning of your meal (not as dessert). At least one meal a day, preferably dinner, avoid grains (potatoes, rice, wheat (bread)) and avoid sugar, especially artificial sugars.
It is recommended to have several meals per day. Having multiple meals per day will help diabetics in maintaining optimal glucose blood levels. Since every meal will affect blood glucose levels it is best to break diet down into lighter meals, which in turn means easier regulation of blood glucose. In diabetes, the pancreas either does not produce enough insulin or it produces enough but it is unable to utilize it efficiently.
There are, of course, other factors that influence blood glucose rise and fall that should be taken into account (such as exercise, stress and infection), meaning that a rise in blood glucose it not always due to ingestion of food.
How to lower blood sugar level?
A patient with diabetes is at a 5 times greater risk of developing cardiovascular disease than patient without diabetes. One third of all cardiovascular diseases also affect people with diabetes.
Three quarters of diabetics die from cardiovascular disease. Women with diabetes have a 4 times greater risk of death from cardiovascular disease. People suffering from diabetes usually have high cholesterol levels as well.
Disturbances in the metabolism of blood sugar levels are mainly the consequence of heredity (diabetes in the family), age (over 40), poor diet, excessive body weight (obesity) and physical inactivity. Disturbances in the metabolism of blood sugar were present in 20% of adult Europeans during 2002-2005 a study showed.
RECOMMENDATIONS to decrease elevated blood sugar:
Blood sugar level is determined in the fasting state. In a healthy person, a normal blood glucose level is less than 108 mg/dL or 6 mmol/L on an empty stomach.
Possible values are
- normal blood sugar level (the blood glucose level is normal on an empty stomach),
- disruption of glycemia (blood glucose in the blood on an empty stomach is increased to a maximum value between 110 and 124 mg/dL (6.1 and 6.9 mmol/L),
- diabetes (elevated blood sugar levels to 126 mg/dL / 7.0 mmol/L or more).
What can you do to lower the chance of developing diabetes:
- lose weight – be fit,
- sleep more, be rested.
- have a healthy diet (read how should a diabetic diet look like) with as many vegetables and fruits, a lot of fiber, consume less calories, less fat, less alcoholic beverages and no simple sugars,
- workout at least 30 minutes per day.
Useful resource: blood sugar levels chart:

American Diabetes Association (ADA) – http://www.diabetes.org/
Children with Diabetes – http://www.childrenwithdiabetes.com/
National Heart, Lung, and Blood Institute – http://www.nhlbi.nih.gov/
International Diabetes Federation – http://www.idf.org/
CDC on Diabetes – http://www.cdc.gov/diabetes/
American Association of Diabetes Educators – http://www.diabeteseducator.org/








































Hallo I check my blood sugar result is 39 I feel dizzy and I don’t know if it s normal or low sugar the nurse just said is normal but I still feel dizzy
39 mg/dl is too low. The minimum should be 70 mg/dl. Lower blood sugar level is one of the primary reason for dizziness. Have some sugar intake to increase the sugar level.
I have been diagnosed prediabetes and insulin resistance recently ,i am verweight and my bloodsug. Levels were from 125 to 140 ml/dl , and 2 weeks ago i bought apple cider vinegar cloudy and unfiltered and bitter melon and dandelion extract, today every morning i measure 100 ml/dl in the morning , after meal aprox 120 and i am happy, regards from Croatia
my age is 20 I check My blood glucose level fasting is 158 pp is 125 its is risk of Diabetes
fasting sugar is high more than 158 postprandial is less than 120 is normal my age is 20
Well one thing is certain. The western diet and lifestyle are making us unhealthy as a nation. What\’s wrong is very simple – processed food loaded with sugar and simple carbohydrates – you know, the cheap ingredients. Get rid of the processed foods and sugar and I think it\’s safe to say we\’d all be much healthier. But the government subsidizes sugar and the mono agriculture of corn, wheat, soy, etc. so that all cheap foods contain these \”cheap\” ingredients. They aren\’t so cheap after all if it makes us all sick with chronic illness and ill health. That\’s why we spend 20% of our GDP on health care. I wonder how much we\’d spend if we were healthy people?
Wouldn\’t it be great if the government subsidized nutritious foods instead? What if there was a \”food\” tax on those food \”products\” that had little-to-no nutritional value – to pay for health care for all? I know, I\’m dreaming……
Hello, i have high blood sugar. What do you recommend to lower it permanently? I suppose there is no easy solution to this, however I\’m keen to know more.
Thank you. Alicia
Sir my fasting sugar level is 52. What to do.
sir my blood sugar is 137mgl/dl at fasting time . night 10- pm
Hello my father sugar levels are
Before breakfast 120
After breakfast 170
Please comment
Hello, was just wondering as to what is normal blood sugar level for non diabetic as opposed to normal blood sugar level for diabetic (if there is such a thing as \”normal\” blood sugar level for diabetic). I hope my question make sense…
Dennis
My bs fasting is 101 and eating then after 2 hours pp is 64 .pls suggest.
My Aunty\’s age is 60. Sugar level is fasting 150. Please tell me some solution.
Any help,
I went for a CBC my Random Blood Glucose is 12.4 mg/dl. The doctor told me to do another test that will be my HBA1C and the result is 6.2% what is that means? any help
Thank you…
this is sanjeev.. i dint had food for 30 hours . in between i had only 2.5 ltr water only. after 30 hours i checked my sugar level its 122.. is it normal blood sugar?
MY BLOOD SUGAR WAS 129 THIS MORNING SOME TIMES IN THE 30S ONCE IN A WHILE BELOW 100 THE REST OF THE DAY SEEMS TO BE OK MY 90 DAY AVE. GLUCOSE IS 136 SHOULD I BE CONCERNED?
Yes, your getting ready to kick the bucket .
My glucose is fbs 21.8 mmo 111
My mom age 44 .sugar level is fasting136.but feet burning very high.plz tell me some solution.
my blood sugar level 6.2 need take medicine ?
Pls advise.
BR
Neshan.
My husband has diabetes but won\’t take his medication his reading arm is 13 he has bad atomic pain
dear sir what is the sugar level in pregnency
I am 66 years old and had total gatrectomy done for NHL in stomach in the year 2000. My blodd sugar readings are eratic and range from 140 (fasting) to 300 (random). I do take insulin (long acting) once in the morning and Glucophage 750 mg once in the evening as per doctor\’s advice. My surgeon who did the total gastrectomy says that upto 200 is ok for my age. Am I a type 1 or 2?
Hi Sir my BS level is 142 fasting pl. Suggest me how can low low my sugar level
Thanx
my sugar level was 3.6 on Saturday my head feels very dizzy it feels like I\’m floating I\’m 29 years old
Is it possible to get any graphical method of say weekly or some times 10 days irregular days with NORMAL graphical line.Soas to check and be precautionary by diabetic patient itself.
Dear Sir,
my age is 52 and my sugar level is 229 so plz suggest me my sugar level normal or exceeded .
sir,my child is 2 years old , his serum glucose level fasting for 8 hours is 96 mg / dl its normal or i must follow him. Tank you
Sir, My suger level is fasting 175 or pp 260 pls tell me how can low my suger level pls… Thank you
Sir my blood sugar fasting 73 or pp 114 pls comment on this report its ok leavel or not
its ok
sir my blood sugar is 136mgl/dl at fasting time .
if your blood sugar is 180 or more, uh, I would go see a doctor. Definitely cut out the sweets, and especially the sodas but really you need to be controlling carb intake because carbs are sugar.
Chromium will lower blood sugar. It is the only thing I have found that will. Do not use it though, unless you are monitoring your blood sugar levels and are already familiar with what those levels are.
please can you tell me why my blood sugar goes between 3and 12
I almost put myself at risk, luckily I went for check up early and my blood sugar levels was 12.9 and when go back after one week it was 8.2. I thank my Dr. because he advised me well to stop drinking fizz drinks, do regular exercise, eat more fruits and vegetables and have a balance diet and I followed the instructions. Now it’s at normal
8.2 is still too high. I have full blown diabetes and I never get readings that high
Hi was wondering could you tell me what the normal blood test should read it’s just my 4 yr old son has autism and recently he had to have a lot of blood tests done for medical and metabolic testing the result is as follows ph 7.378 pco2 5.09kpa po2 11.24kpa hit 38.3 percent na’137.6mmol/l k’3.97mmol/ l ca2+1.187mmol/l glu 5.9mmol/l lac1.8mmol/l uhb12.5g/dl be _277 mmol/l chco2 22.0 mmo/l so2 97.0percent O2 he 95.5 percent Cohb0.9 percent methb0.6 percent hub 3.0 percent and Bill value below 3.0 mg /dl are these ok or should I be worried haven’t to go back to drs fir 2 months
I was hospitalized for 6 days, brought in with blood sugar of 14 and body temp 91. I have been taking my readings every morning since I have been released (about 2 weeks) my Blood has been back in forth from 60 to 89 but this morning I didn’t wake up til 11:30 am and it was 138! This is on an empty stomach. Is this just as bad as being dreadfully low? We still have no answers as of why it was at 14.
My wife 69 years old diabetic for 27 years.from 9 a.m. To midnight her Blood sugar is in Hyperglycemia range, mostly in the range 250/350 mg/DL.After midnight her Blood Sugar level drops at a very high rate and by 3/4 a.m. It drops to Hypoglycemia range,mostly in the range 40/80 mg/DL. After 5 a.m. It starts reversing and by 7 a.m. It shows her Blood Sugar level in normal range say 100/110 mg/DL.
This is inspite of the fact that she is not given any medicine after lunch and no food after 10p.m.
Can anybody tell from where insulin comes after midnight and from where sugar comes after 5 a.m.?
blood sugars rise at night because of cortisol levels. The high sugars at night are common. The numbers you mentioned during the day are very high. Speak with your doctor. You might need to check your blood glucose before meals and get insulin coverage for meals. She needs a doctor.
My uncle who is 65 yes old having diabetes. His sugar level during fasting is 148 mg/dl and after 2 hours from mealbit is 258 mg/DL. Please suggest what to do?
I recently checked my blood sugar out of curiosity and it was 49 mg/dL. I felt completely normal though. I’m 17 years old, 4’11 and 105 lbs. I have had symptoms of hypoglycemia in the past (dizziness, increased heart rate, fatigue), but overall, I’m a very healthy individual. My mother has low blood sugar levels, as well, but she’s never experienced this. I must also add that my father is a diabetic (which explains why i have a blood glucose tester) and diabetes runs in my family. I don’t have diabetes, however. So… can anyone explain what’s going on with my blood sugar?!
A fasting reading this morning I did was 83 then I ate and checked again after and hour or so it was 110. Then checked again at random it was 96. My doc suggested I might be hypoglycemic because of some of the particular symptoms I’ve had. I’m not sure if my sugar just runs low because most of the time I don’t feel the symptoms. But when I do I get scared out of my wits. I don’t scare easily so I know this is nothing to be messed with. Idk know what my normal sugar level is being that I’m 6’6 148lbs
My normal blood sugar reading is between 102 to 110 before breakfast my goal is to keep it from going any higher 126 in the morning before breakfast is high to me .I am type 2 diabetic. I watches what I eat and exercise when I can walking is good
My random blood sugar was 103 is that normal?? Plz reply
sir i check my blood sugar level in the morning after 2hr of taking meal. it showing 103 mg/dl. what it show. i am 23yr old. & my father has diabetes problem. he give me blood in my child hood when i admitted in hospital that time i was 2 yrs old. is their possibility that i also have diabetes problem.
please help me, guided me.
in the hope of favorable response
thank you.
Just around the borderline on both BP and Blood Sugar. Learning how to use natural means (diet and exercise) to keep both within normal ranges.
sir now a days my blood suger level is high after meal my suger in night 183 and after drink tea is 153 and i do not eat sweet and drink then my suger level is high my age is just 24 my 6 month beby and my family heredity blood suger
Hi
In the morning 6.2 is that bad ?
What can i do to lower this #
Thanks
Nigel Smith, look at what you are eating in the morning and try something with a bit more fibre. This should take a bit longer for the sugar to get into your blood. Sometimes with exercise, glucagon is produced by your liver if your blood sugar is too low and this will increase the test result. Only you know what you have eaten so diet is important. Speak to your doctor for diet advice.
🙂
Karon
Thank you. In the morning I tend to just have porridge oats with skimmed milk. My higher readings tend to be pre breakfast although the levels are coming down. Regrettably I have found that diabetes nurses have just told me that diabetes is a function of previous smoking ( I never have) and I am over weight ( I’m not) so I am lacking confidence in their ability to view me as an individual and advise accordingly.
Thank you for your guidance. Gratefully received
Nigel
Excellent site
Being new to this, and someone who does not do things by halves, I have been tracking my glucose levels some 4 or 5 times a day. It appears that c1 hour after waking my results are the highest, 7.5-9 mol/l. Rest of day always below 7 with an average for the day of 6.5-7mmol/l. I eat healthily and am not overweight , go to gym etc
How can I bring down my morning reading as this will reduce the average to closer to 6.25/6.5?
Are my results a problem?
Thanks
Nigel
Apologies
All figures in above should be mmol/l
Very informative article
My blood sugar level is 100mg/dl. What are the preventive measures taken at this level ?
I need an solution for decreasing sugar level from 190mg/dl
to safe zone…please help me ….
age of patient is 50years..
thank you alot..
I got a fasting blood glucose test done for my 10 year old son. The result was 106mg/dl. As per your website, it states that fasting levels till 180 for his age group are fine whereas other websites like Wikipedia and Mayo clinic state that 100-125 is pre-diabetic. Would you please explain why is there so much of a difference and which one should I actually believe in? I am really worried. Please help.
SORY ABOUT SPELING I NEVE COOD.i was told by doctors 9 muths ago I had tipy 2 and givin metermothin 500mg 4 times a day ime falling asleep in the afternoon as ime finding it hard to keep awake can eney one help.
if my fathers (age 57)all check up values are normal only sugar value before lunch is153 and after lunch is 307.is it possible?or report is wrong.should i do check up once again.
my mean blood sugar value for fasting is 134.5 and that of random is 156.5
however my HbA1c is 6.4
kindly guide me whether i am pre-diabetic or diabetic ?
Well I’m a tattoo artist and also overweight I’m 5’6 and weigh 250 lbs been heavy my whole life and have been noticing I’ve been more thirsty and also urinating more often . I don’t have medical coverage so I decided to go but a glucose meter and check levels today I haven’t ate in 8 hrs and took test this morning and it said 232mg so now I’m a lil worried and hopeing if I can start eating better and exercise more I can bring it down some being a tattoo artist I’m sitting down all the time all day drawing designs and tattooing for sometimes 8 hrs or more any advice to helpaybe with diet and or exercises would be helpful thanks for any reply …
We randomly test my 4 year old daughters glucose and it has never been under 7 mmol/L. Yesterday morning it was 7.8 so we didn’t give her anything else to eat but some cinamon water to drink, and this morning on an empty stomach the reading was 7.1 mmol/ L We gave her some plain oatmeal after the test. Is there reason for concern. My family has a strong history of diabetes and I had gestational diabetes with her brother and sister, but not when I was pregnant with her.
My 6 year old son was recently diagnosed as pre-diabetic. He is 4 ft tall and weighs 48lbs so as you can tell he is not over weight in fact his height and weight are perfectly proportionate to each other. Any way the doctor just called me and told me that his blood glucose levels are high but his insulin levels are normal. The only information she gave me was to change his diet and get the levels checked again in three months. Is that a normal response or is there something else I need to be doing. I have no ideal what the numbers said and I’m just really confused.
Hi there
my sugar level in the early morning is 6.1 to 6.8 just in the early morning . During the day and after lunch in 2 hours never above 6 .What does that mean .
Any thing to worry about
Is it high # if so
What can i do to avoid the high # in the morning.
Thanks
Thanks for the info, but now I’m confused. I went to a healthy heart clinic and now my doctor wants me to have another test. I have an appointment for a HBA1C test, my doctor said it’s just routine (I am not diabetic). I assume they think I could be diabetic (my mother is type 2). I did a fasting test which came out at 6.1, but then I did another test after 2 hours from eating (apple pie & ice cream), this came out at 12.9. What does this mean? Looking at what I’m reading on websites, it means I’m diabetic, but then I’m not? Please can anyone explain.
Your values may indicate pre-diabetes. Given the fact that your mother has type 2 diabetes you are under greater risk to develop diabetes type 2 as well (although this relation has never been confirmed by scientists). But we cannot diagnose you, only your personal doctor can do that.
What you can do is to change your diet and delay the possible development of this disease by following some simple diet rules. Read more here: //healthiack.com/diets/diet-for-people-with-diabetes
Thanks for that. I know it recommends that you eat fruit, but my mother’s blood sugar only got under control after she stopped eating fruit?
A person with diabetes can enjoy all fruits – be it pineapple or cherries, apples or figs …even citrus fruits and grapes. The only limitation is the amount of fruits eaten. This amount is different for every person. Your mother’s case is somehow odd as fruit is recommended food for diabetics.
The following two lines from your table do not make sense. Postprandial blood glucose levels should be higher not lower than random blood sugar levels.
about 70-125 mg/dl (3.9-6.9 mmol/l) Normal random blood sugar
about 70-111 mg/dl (3.9-6.2 mmol/l) Normal postprandial blood sugar
Are they switched? Or does one have an error?
Thank you for pointing that out. There was a slight typo in the chart.
Normal postprandial blood sugar level is between 70 and 199 mg/dl or 3.9 to 10.9 mmol/l where 199 mg/dl (10.9 mmol/l) is a borderline value and may already indicate diabetes.
I am 48y I test my blood levels at morning some times it is 89 some normaly 95 99 some times it is 103 after meals 1 h it 134 155 165 but after 2 h it is 100 107 some times it is 118 not lot do I consider my self normal or predicated I ckecked my levels for 3 months accumulating it was 5.2 and now after some diet and exercise it is 4.3
A random test of blood sugar at 1 pm showed 230. Had breakfast at 10 am. Age 28 Male.
Fasting sugar 91 and after eating meal it is 83.age 45 male
When I got first diagnosed, my BG was 828. I was normal but because I lost lots of weight and felt too thirsty and urinate frequently, I went to see a doctor. Then he put me in medication. I am too glad that I did not end up in coma.
best site I have seen
So – one doctor tells me I am prediabetic with fasting level 5.8 and another says no way! yet….I know I am sugar sensitive….what do I do???
In my opinion it is always best to get more opinions. Go see another doctor. 5.8 value may indicate prediabetes.
Marco
Dears Site Organizer,
The content of the site you provided with the considerable information is so well arranged to benefit the users , specially those who are seeking the knowledge to check themselves with the diabetics particulars to be helped accordingly.
I suggest to develop your site to be linked with the new diabetic’s Instruments as I hope the testing Unites will be produced which does not need to prick fingers for the Blood testing .
Over all I really enjoyed to go through the site and the data furnished . Thank You.
hi, i was diagnosed with type 2 diabeties, and have not been taking my medication regularly. I did my HBA1C about 3 weeks back, and the result was 14mmol/l. Well, now i have been constantly on medication and its currently in the range of 5-8mmol/l. This is for before food (took the reading for before breakfast and dinner, but not lunch). Yes i tracked them.
But my question is, after been on “sugar” for quite some time, and now in the process of lowering the blood sugar level, i hav efound myself to be giddy, like really bad headaches but not migraines. Sometimes as though i feel that what i am seeing is actually a dream, that its not real.
And when that happens, i check my blood pressure is normal, and my glucose reading will be between 5 to 5.5 mmol/l.
Is this normal or should be expected by me during this phase of “recovery”? Is there anyone that could advise me please?
Really appreciate it.
Btw, i dont feel thirsty or inceased urination. Although my eyesight is not sharp as it used to be.
As a nurse and parent of a type 1 diabetic child, your numbers are way off. Nothing under a 4.0 is normal. Anything under 4.0 requires fast acting sugar. Low blood sugar can cause serious damage. Please be more responsible with your “facts”.
If anyone is in doubt, please seek treatment. Especially if there is increased thirst, urination and weight loss. Vomiting and lethargy are a huge indication to seek ambulatory treatment if combined with the other symptoms.
authorities confirmed these information?
Values are accurate. For conversion between mmol/l and mg/dl use our blood sugar converter.
What is normal blood sugar level
My mom has type 2 diabetes, and has a lot of trouble regulating her levels, she is 79
I thought as I was testing hers I’d do mine. I just eaten about 10 mins and my results were 9.0 is that high I suffer with high blood pressure and I’m 53.
I have been a constant dull headache on my forehead for the past 3 weeks with intermittent nausea. My doctor ordered a CBC and thyroid test. Everything came back WNL except my glucose was 64. This was a random glucose. I had eaten breakfast 3 hrs before the test. My doctor is not concerned with my result. Could the low blood sugar be causing my symptoms? I am otherwise a healthy 34 feamle.
it would be highly appreciated if you could give me a chart including glucose amount of various food and vegetables.my fasting blood sugar test is 109 and I really afraid of that .
how can i convert mmol to mg. unit
Feel free to use our blood sugar converter.
i like this page it is hard to find a page like this that tells every thing about to were u understand
I went to doctor, had tetanus shot, 9 days later ended up in emergency room, spent 2 days in ICU with blood sugar level of 1700. Now diagnosed with type 2. No one in family has diabetes. Could vaccines do this?
Hi ,My mother went for random blood glucose level test…. Result says its 234mg/dL …. May I knw,wat is her present condition???? Is it controllable???My mom’s age is 50yrs…. Plz do rply asap 🙁
Your figures are not consistent – sometimes you say that up to 5.5 is a ‘normal’ fasting glucose (true) and then about 2 sentences later you say that it is anything up to 6.1 (no – that’s impaired fasting glycaemia) but you state at least 3 different numbers for ‘normal’ fasting. Also I think your figures for children are wildly off.
Hallow,my sugar level 4hours after eating was 3.9 and in the morning before eating was 4.5 ,is there with problem with me?kindly advice
80 years old and blood sugar before breakfast runs between 140 and 160. Is that within a normal range.
You are way above the normal range.What is your weight and what do you think is a good weight if you could be? What kind of foods do you normally eat? Fat in the cells is the main contributer to type 2 diabetes.Your doctor should put you on Metforman,the best most widely used diabetic med in the world.Undoubtly need to lose weight, change your eating habits more walking etc. what ever it takes to get diabetes under control. Please do something about it. Don
This portion of information on blood glucose is very helpful and positive. Keep up the good work on health tips. God bless you.
very helpful, but there is no answers to the questions
Hi Dear,
I have checked my sugar with empty stomach FBS-135, is it helthy or else diabates.
pLease let me know .
My daughter has been having all the symptoms of low blood sugar. So I borrowed my mother in laws meter to check when she has an episode. Fasting it is 95. Is that normal for a 10 year old girl first thing in the morning?
this article is spot on. thanks a lot
I have hypoglycemic symptoms that’s why my doctor gave me a glucometer to check my blood sugar regularly. I have a question : In the morning on a empty stomach my blood sugar was at 4.7mmol on the glucometer. two hours after a tuna sandwich I went at 6.5mmol and later in the day after a meal I was at 6.4 mmol. I noticed that if I eat a good quality meal with veggies, lean meat and whole wheat pastas my mmol are around 6.4-6.5 and if I eat something cheap like from a fastfood or something like a sandwich without proper ingredients my blood sugar stays around 4.9mmol. Is this normal?
I need to eat regularly and healty which I started doing. Are my readings alright?
Oops I meant his Dad is a Type 1 Diabetic in my previous post . Not Type 2.
My 2 1/2 year old who is potty trained recently started having random accidents. I noticed an increase in his daily times he urinates. His school noticed today also that he voided 6 times at school today and had two accidents. This prompted me to check his sugar once we got home and his random sugar today was 180. Not sure if I am worried over nothing but I am gonna get his urine checked in the morning. His dad is a type 2 diabetic. Also thought about a UTI.
my grandsons fasting bloodsugar was 3.8 , is this a concern and should we check with Dr.
Both his maternal grandmothers have type 1 diabetes
sir my age is 28 and i examined the blood sugar level .my fasting level is 80 and after meal(postmeal) 150. may it indicates dibetics case.
fasting level is normal…… and you don’t say how long post meal or what you ate. Although it is said that most people doing rise much above 140 after meals, so yours is hardly way out of whack. Also, it is better to have an A1C test… because it tests your blood sugar over a longer course…. spot checking doesn’t give you anything but a snapshot in time. Obviously if you are a diabetic, yeah, test yourself especially when you are trying to find out if there’s foods you should avoid…..
I was diagnosed with Type2 Diabetes in May and the result was 94 ,I have since had another Test and have been told that it has come down to 47,I have been following a strict Diet of no Sugar and trying to not have Carbohydrates although have had Brown Pasta and Seeded Wholemeal Bread,I eat meat,chicken and Fish ,Salads,Green Vegetables non acidic Fruits,I drink water Soya Milk and try to have regular medium meals and I have lost weight and I am now within the weight for my height and I exercise everyday and try not to sit about for long but I do not see the levels shown here in the form I have been given and the Nurse did not mention having to take Medication which I was trying so hard to avoid so are my readings ok?
I am recently diagnosed with Diabetes with Fasting Glucose test of 7.9 before suggary drink and 16.3 at 2 hours after. But, since then I started working out at the gym and changed to a low carb diet. Now it reads 6.2 before meals and 6.8 at 2 hours after meals. Should i take the precribed medication. I haven’t taken yet.
Although your readings appear to be much better, you should still follow your doctor’s suggestion. We cannot give you medical advice, only your doctor can. Consult your doctor and stay on the safe side.
I have 140 to 165 .does it indicate i have diabetes
my fasting sugar level is 122 is it ok or not
Your value might indicate pre-diabetes. For more reliable result please repeat measuring in fasting state. Consult your personal doctor when in doubt!
prediabetes!!! You should be under 80 -100
in fasting.
i am new at this diabetes and i don’t undestand diabetes.early in the morning my blood sugar sometime in the 90’s may be 100 some mornings.and during the day 122 never 200. need a site i can go to help undestand diabetes and a chart to go by.
Consult your doctor for more information.
Diabetes is characterized as chronically elevated blood glucose (blood sugar) which your body needs for energy. This occurs whether because the pancreas is not providing sufficient amount of insulin (diabetes type I) or target tissues are not responding to insulin (type II diabetes). Diabetes is more likely to develop in families with known diabetes history.
Blood sugar level chart:
less than 6.1 (140) on an empty stomach means normal value, between 6.1 (140) and 6.9 (169) on an empty stomach indicates a limit value, more than 7.0 (172) on an empty stomach could mean possible diabetes and more than 11.0 (260) anytime usually indicates diabetes.
I have been transformed by your information….may God direct you the more so that we can benefit more from your rich information
after view your web site I satisfied lot
thanks
very good, specific information.
my sugar level some time low some time high is going from fasting 5.5-6.8 and after eating 1h is 8.5 and after 3 h is going back 5.8 thanks
Is there a problem brewing if glucose levels are below 60 more than 4 times a month? What should the range be during the day, 100 to 160? How long does the blood sugar have to be below say 140 each day? I have type II diabetes.
IS there any difference in adult and children’s sugar level ???
Expected values differs a bit as children’s blood sugar levels are often slightly lower than adults.
my blood sugar level is after fasting 126 , and after food is 166 whether I am Diabetics pls.explain
blood test 120 mg dl is this ok
Yes, that number is quite good. Is that before or after eating? Usually you want numbers between 70 to 120. I have type 1 diabetes. I have had it since the age of 24.
Very informative – thank you so much
I have type 1 diabetes and I find this information and
chart very helpful.
John B Harrison
sir sugar level some time low some time high..